#17 Traumatic Shoulder Instability with Hamish Macauley


/
RSS Feed
- Hamish's thoughts on his experiences working as a head Physio in both professional rugby and the AFL
- What to expect from Hamish at the Upper Limb Rehabilitation in Sport course in the Gold Coast
- Posterior dislocation- what are the tell tale signs?
- Where early management is different between posterior & anterior dislocations
- Common imaging findings following both posterior & anterior shoulder dislocations
- Decision making around surgical Vs non surgical management following instability episodes (see further detailed notes below)
- Differences in post surgical management for anterior and posterior repairs
- Post surgical rehabilitation
- Early exercises & targets
- Time based expectations on restoring ROM and strength
- How & when to introduce pushing, pulling and over head
- How and when to take the athlete into venerable positions (Abd/ ER
- Testing or benchmarking in readiness for a return to play
- What is often missed in shoulder rehabilitation
- Contact based conditioning
- Occupation: overhead/manual labour vs sedentary
- Sporting demands – collision sports
- Co-morbidities/physical inactivity – prolongs recovery
- Evidence based surgical indications (reduces the chance of recurrence): Male <25 y/o with traumatic MOI, requires relocation + high functional demands = EBP supports surgical repair. Generally the risk factors from the literature for recurrent instability include: young age (<40 = 13x higher; majority occurring <25), being a male, contact sport. I would also include young females in collision sports in this category. However it is a discussion and as we discussed there is evidence that people in this group can have a positive outcome without surgery.
- Hypermobility:
- I always question the patient about their episode(s) – patients can use the words dislocation and subluxation synonymously. True dislocation or instability in the absence of dislocation. I always I always question the patient around the MOI and do they have imaging evidence of the dislocation (in ED)/needed someone to relocate the shoulder… If their story is accurate for the MOI then I generally believe them when they say their shoulder dislocated. If they haven’t had true dislocation, rather instability episodes – conservative treatment. Especially if you’re dealing with someone who has more mobility than the average (>4 Beighton’s).
- Traditional classification include the TUBS (Traumatic, unilateral, Bankart, Surgery) and AMBRI (Atraumatic, Multidirectional instability, Bilateral, Recurrent, Inferior Capsular Shift), however this 2nd population doesn’t do as well with surgery as was initially intended with this classification, so conservative path is the best here. A further classification system – The Stanmore Classification (diagram below) further stratifies it into 3 groups and the relationship between trauma, structure and muscle patterning – article attached. In short, group I relates to traumatic dislocation and structural failure, group II with structural laxity that can pre-dispose them to instability with or without trauma, group III to muscle patterning issues causing instability/resting subluxation. Surgery is indicated in group I and only considered in group II with structural failure and who have failed a good rehab program.
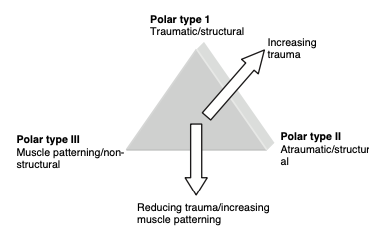 Reference article: Jaggi & Lanbert 2010, Rehabilitation for Shoulder Instability
Reference article: Jaggi & Lanbert 2010, Rehabilitation for Shoulder InstabilityOther Episodes
Storytelling in business has become a field in its own right as industries have grown

#24 Physiotherapist’s Role in Acute High-Trauma Including Life-Threatening Injuries with Gina Nelson
In this 24th episode of the Sports MAP Podcast we chat with Director & Head Physio of Q Performance, Gina Nelson. Gina has over 8 […]
Listen Now
#19 Physical Qualities required to Perform in Formula 1 with Kim Keedle
In this 19th episode of the Sports Podcast we chat to Formula 1 Physiotherapist & Performance coach Kim Keedle on the physical requirements and preparation […]
Listen Now
#22 Managing Return to Play from Concussion with Laura Fazzari
In this 22nd episode of the Sports MAP Podcast we chat with St Kilda Football Club Physiotherapist and concussion expert Laura Fazzari. Laura also works […]
Listen Now